Post-Inflammatory Hyperpigmentation and Chemical Peel Strategies
Post-inflammatory hyperpigmentation is a reactive pigment disorder that follows cutaneous inflammation or injury. Successful peel planning requires control, restraint, phototype awareness, and a strategy centered on pigment stability rather than excessive aggression.

Clinical close-up illustrating reactive hyperpigmentation after prior cutaneous inflammation.
Clinical Understanding of Post-Inflammatory Hyperpigmentation
PIH develops when inflammation stimulates melanocyte activity or causes pigmentary disruption after acne, eczema, friction, procedures, burns, or other cutaneous injury.
Post-inflammatory hyperpigmentation is not a primary pigment disease in itself, but a secondary response to skin aggression. The pigmentation may be epidermal, dermal, or mixed, and its persistence depends on the depth of inflammation, the phototype, and the adequacy of subsequent care.
In aesthetic practice, PIH is highly relevant because it may follow both spontaneous inflammatory skin disease and poorly controlled procedures. This is why peel selection must remain indication-based and should never ignore the biology of reactive pigmentation.
- Triggered by prior inflammation or irritation
- Common after acne and procedural trauma
- More persistent in higher phototypes
- Requires pigment-safe treatment planning

Why PIH Deserves a Dedicated Clinical Strategy
PIH is often underestimated, yet it is one of the most frequent causes of dissatisfaction after inflammation or poorly adapted procedures.
◐
It Can Last
PIH may persist for months when the inflammatory signal is strong or when treatment restarts irritation instead of calming pigment activity.
◎
It Is Reactive
Aggressive treatment may worsen reactive pigmentation, especially in skin already sensitized by acne, friction, eczema, or prior procedures.
⚠
It Needs Restraint
The goal is not to chase rapid peeling, but to reduce inflammation, stabilize melanocyte activity, and progressively normalize skin tone.
Pathophysiology and Pigment Logic
PIH reflects a cascade linking inflammation, mediator release, melanocyte stimulation, and pigment deposition.
Inflammatory mediators such as prostaglandins, leukotrienes, cytokines, and oxidative stress signals stimulate melanogenesis. When the epidermis is disrupted more deeply, pigment may also drop into the dermis, where clearance becomes slower and more difficult.
This explains why superficial color improvement may be easier in epidermal PIH than in mixed or dermal presentations. It also explains why controlling inflammation is as important as selecting the acid itself.
- Inflammation upregulates melanocyte activity
- Oxidative stress amplifies pigment signaling
- Barrier disruption increases reactivity
- Dermal pigment takes longer to fade
Inflammation First
Pigment appears after prior skin aggression, not in isolation.
Melanocyte Response
Reactive melanogenesis intensifies discoloration after injury.
Depth Matters
Epidermal and dermal pigment do not respond with the same speed or predictability.
For this reason, rational PIH treatment combines anti-inflammatory logic, pigment modulation, and careful procedural sequencing.
Main Risk Profiles in PIH
Some clinical contexts are particularly prone to pigment instability and require stricter control.
Acne-Related PIH
Very common after inflammatory acne, excoriation, and repeated irritation in adolescents and adults.
Procedure-Induced PIH
May follow lasers, overly aggressive peels, frictional treatments, or insufficient photoprotection.
Higher Phototypes
Darker skin tones require particular caution because melanocyte reactivity and pigment persistence are often greater.
Skin of color, recent inflammation, active picking, barrier impairment, and repeated irritation all increase the need for a conservative protocol design.
Product Integration for PIH Management
Product selection should calm reactivity, support pigment regulation, and help avoid rebound inflammation.

Pigment Support
Clarté de Lune
Relevant when PIH requires supportive pigment modulation, a calmer maintenance phase, and a more controlled correction logic.
- Supportive tone regulation
- Maintenance-oriented logic
- Useful in pigment instability

Preparation Phase
Gradient Cream
Useful for progressive preparation, tolerance building, and gentle protocol escalation when the skin is easily irritated or pigment-reactive.
- Progressive introduction logic
- Helps reduce abrupt irritation
- Supports cautious sequencing

Supportive Regulation
Stretchpeel
May support long-term pigment management when PIH coexists with recurrent exposure, oxidative stress, or the need for a broader maintenance concept.
- Adjunctive support logic
- Useful in extended maintenance
- Compatible with pigment-focused care
Strategic Treatment Planning for PIH
PIH management should prioritize stabilization, phototype-sensitive progression, and minimization of new inflammation.
In PIH, the best strategy is usually staged and deliberate. Active inflammation should first be reduced, the barrier respected, and the treatment escalated only when the skin demonstrates sufficient stability.
- Identify the original inflammatory trigger
- Assess phototype and pigment persistence risk
- Prefer controlled progression over abrupt intensity
- Combine treatment with long-term pigment-safe maintenance
Main Therapeutic Objectives
- Reduce reactive pigmentation
- Prevent rebound darkening
- Preserve barrier stability
- Promote more even tone over time
Clinical outcomes depend on pigment depth, trigger control, procedural restraint, and adherence to maintenance.
Before / After Strategy
This section should document realistic reduction in visible discoloration and improved tonal harmony while respecting the chronic and reactive nature of PIH.
Before

Baseline appearance showing irregular post-inflammatory brown discoloration following previous cutaneous inflammation.
After

Progressive improvement in tonal homogeneity and visible reduction in residual reactive pigmentation after protocol-based management.
Best practice: use the same lighting, angle, and timing conditions when documenting PIH, because subtle pigment changes are easily distorted by photographic variation.
FAQ
-
What is post-inflammatory hyperpigmentation?
Post-inflammatory hyperpigmentation is a reactive darkening of the skin that appears after inflammation, irritation, acne, procedures, or other forms of cutaneous injury.
-
Is PIH the same as melasma?
No. PIH follows inflammation or irritation, whereas melasma is a chronic pigment disorder with a different pathophysiology and a different treatment logic.
-
Can chemical peels help in PIH?
Yes, but only when selected carefully. In PIH, peel strategy should be conservative, phototype-aware, and designed to avoid renewed inflammation.
-
Why can PIH worsen after treatment?
It may worsen when treatment is too aggressive, when the barrier is already unstable, or when inflammation is reactivated instead of controlled.
-
Is PIH more common in skin of color?
Yes. Higher phototypes tend to show stronger or more persistent reactive pigmentation, which is why preventive and therapeutic caution is especially important.
Related Clinical Topics
Explore related conditions that frequently overlap with PIH or influence pigment-focused treatment design.

Acne
Acne is one of the most frequent triggers of PIH and often determines both the timing and the sequencing of treatment.
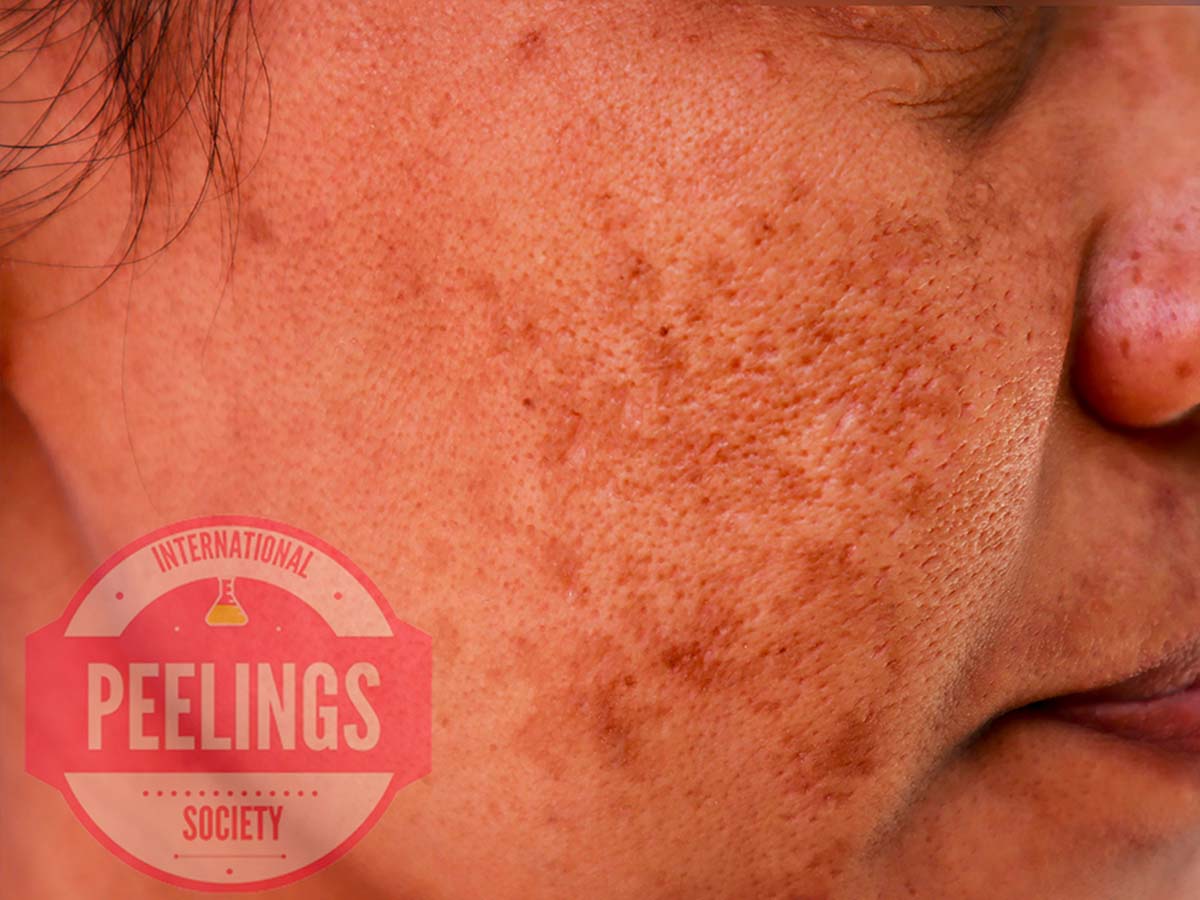
Melasma
Although different from PIH, melasma enters the differential diagnosis whenever facial hyperpigmentation needs structured assessment.
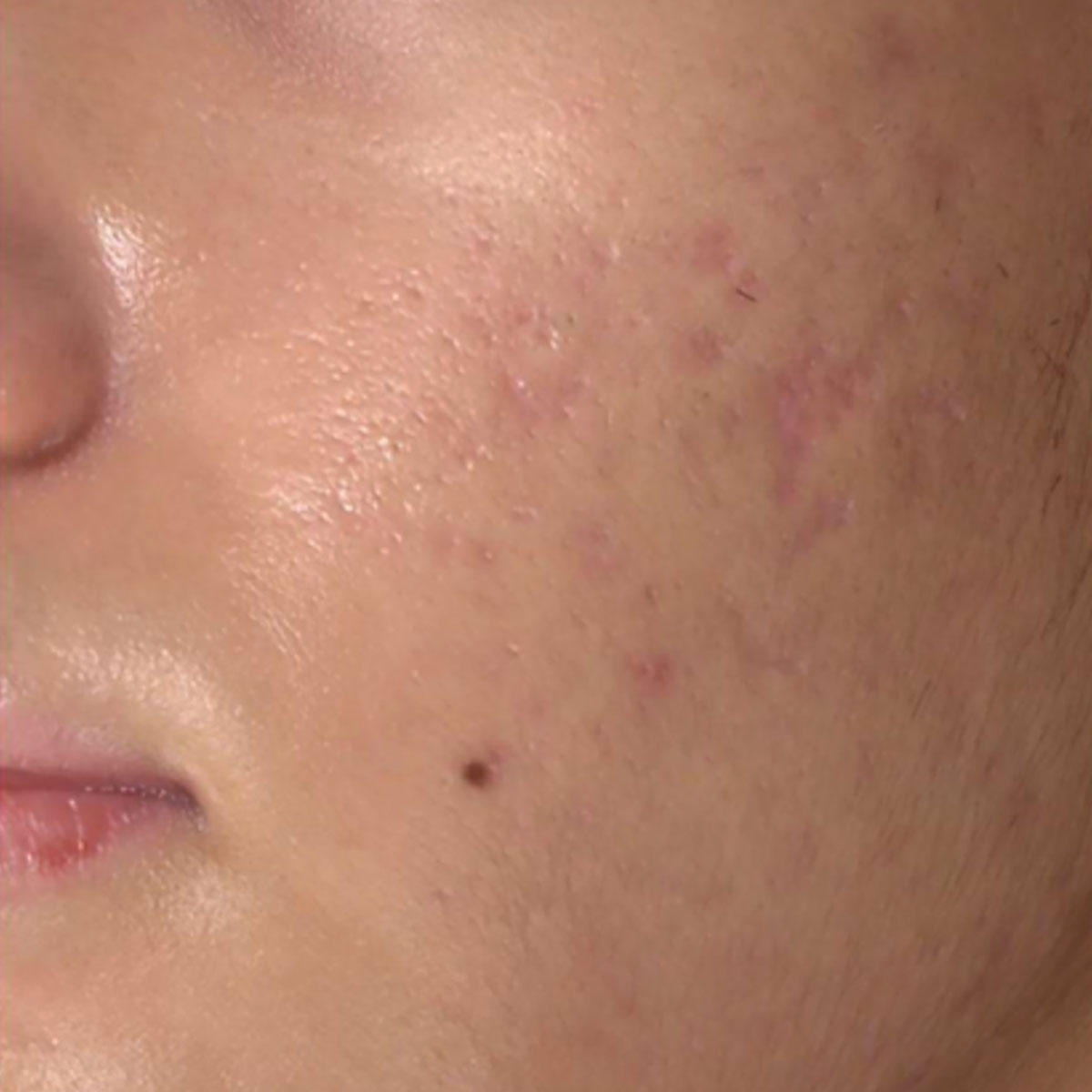
Acne Scars
Scar-focused treatment often carries a risk of reactive pigmentation and therefore requires pigment-aware planning.

Skin of Color
PIH is a central consideration in higher phototypes and should always be integrated into procedural decision-making.
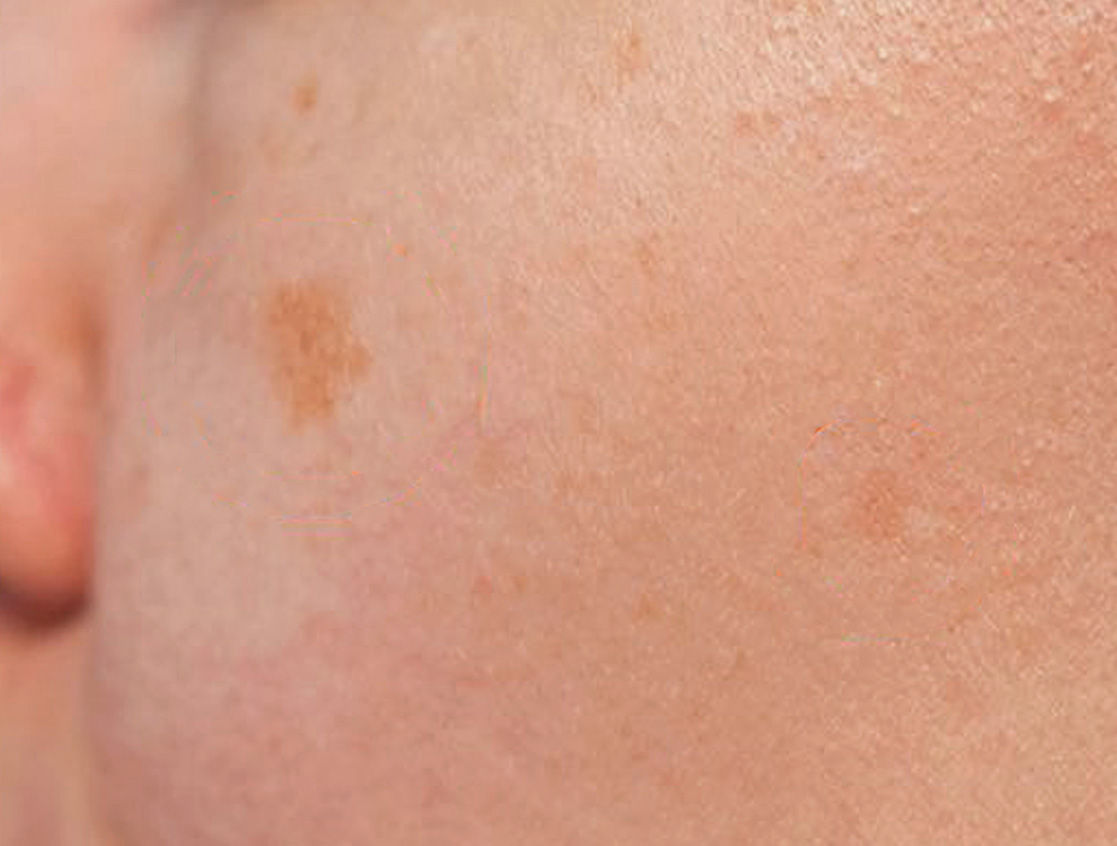
Solar Lentigines
Lentigines and PIH may both appear as brown macules, but their origin and therapeutic management are not identical.
Explore Protocols, Products
and Professional Training
PIH management requires pigment-safe strategy, procedural discipline, and long-term maintenance rather than abrupt or overly aggressive correction.
Continue with dedicated protocols, professional formulations, and training resources designed for practitioners working with reactive pigmentation and post-inflammatory discoloration.

